What Should My Athlete Do After an Injury? How Can They Safely and Quickly Get Back on the Field?
To answer these questions, let’s explore the sports physical therapy process for one of the most common soft tissue injuries in soccer: a quad strain. For more details on soft tissue injuries and the differences between strains and sprains, check out last week’s article here.
Soccer players are prone to soft tissue injuries due to the sport’s high demands of sprinting, kicking, and sharp directional changes. Kicking injuries are particularly common, with the rectus femoris muscle, part of the quadriceps group, being the most frequently injured.
The rectus femoris muscle spans both the hip and knee. When an athlete winds up to kick a soccer ball, this muscle quickly stretches and contracts to execute the kick. Any muscle that repeatedly lengthens and shortens rapidly, especially across multiple joints like the hip and knee, is at a higher risk of injury.
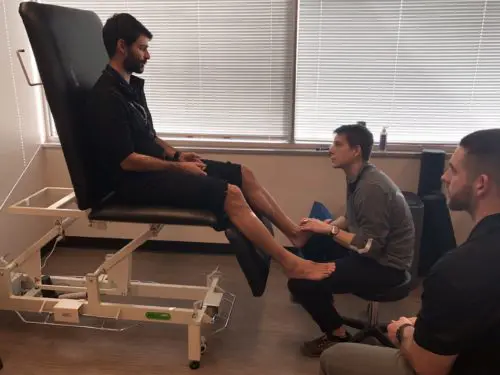
Immediately following an injury, the athlete should be evaluated by a physical therapist or sports medicine physician to assess the severity and determine the appropriate course of action. While imaging can be useful, it’s not always necessary.
The rehabilitation process for a muscle strain can be broken down into three distinct phases:
1. Injury Management Phase
The goals of this phase are to reduce pain and inflammation, restore the muscle’s range of motion, and reintroduce pain-free functional movements. While the injured tissues need time to heal, complete rest isn’t the answer. Light strengthening exercises and mobility drills are essential to stimulate the healing process, making early physical therapy crucial.
Examples of early-phase exercises for a quad strain might include:
– Isometric knee extension with hip extended
– Split squat isometric
– Single-leg bear hold
Once athletes regain a full range of motion without pain and can perform basic bodyweight movements, they move on to the next phase of rehabilitation. Unfortunately, traditional physical therapy often stops here, leaving many athletes struggling to bridge the gap between rehab and full performance.
2. Strength Training Phase
At the beginning of this phase, many athletes still face significant strength deficits.
Strength training is vital for improving the quality of the injured tissue and reducing the risk of reinjury. This is the time to hit the weight room.
Strength training exercises for an athlete recovering from a rectus femoris or quad strain might include:
– Reverse Nordic curls
– Lateral step downs
– Safety squat bar step-ups
3. Sport-Specific Training
What must the injured tissue be able to do for a safe return to sport?
This phase of rehab demands a deep understanding of the athlete’s sport, ensuring the injured area is prepared for the challenges ahead.
Since the rectus femoris is often injured due to continuous, rapid lengthening and shortening, this movement pattern must be replicated and trained during rehab to prepare the athlete for the demands of soccer.
Some examples of exercises used in this phase might include:
– Alternating split squat jumps
– Banded deceleration drills
While these three phases apply to all muscle strains, the recovery timeline varies based on factors such as the injured body part, the severity of the injury, and other individual factors.
If your athlete is dealing with a muscle strain, it’s essential to schedule an appointment with a physical therapist or sports medicine physician as soon as possible. Early treatment has been shown to get athletes back on the field faster and more effectively. If you suspect that you or your child has a muscle strain, schedule an evaluation with us right away.